Bariatric Surgery Treatments
Vertical Sleeve Gastrectomy
Roux-en-Y Gastric Bypass
The gastric bypass surgical technique, which limits food intake and keeps it from being absorbed completely, is a frequently performed bariatric and metabolic procedure in the United States and is the ‘gold standard’ procedure for optimal weight loss and health. This technique alters the way in which your body responds to food. It changes the release of hormones, leading to decreased appetite and reduces overall absorption of calories and nutrients.
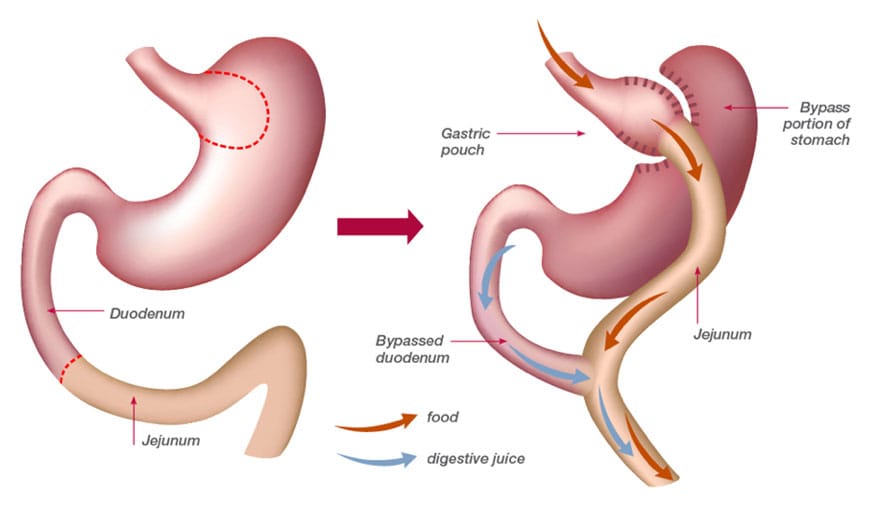
- The pouch is surgically attached to the middle of the small intestine, thereby bypassing the rest of the stomach and the upper portion of the small intestine (duodenum)
- The smaller stomach size helps patients feel full more quickly, which reduces food intake. Bypassing part of the intestine limits calorie absorption
- Gastric bypass also produces positive metabolic changes in many organs as a result
Advantages
- Limits the amount of food that can be eaten at a meal and reduces the desire to eat
- Average excess weight loss is generally higher than with gastric banding or sleeve gastrectomy
- An analysis of clinical studies reported an average excess weight loss of 62% in 4,204 patients.15
- Shown to help resolve type 2 diabetes (68%), high blood pressure (66%), obstructive sleep apnea (76%), and to help improve high cholesterol (95%).1, 16, 17
- In a study of 608 gastric bypass patients, 553 maintained contact for 14 years; the study reported that significant weight loss was maintained at 14 years.18
Risks
- Given the duodenum is bypassed, poor absorption of iron and calcium can result in the lowering of total body iron and a predisposition to iron deficiency anemia. All patients should be aware of the potential for heightened bone calcium loss. Baseline DEXA is recommended for all postmenopausal women after weight loss surgery, men 70 years and older after weight loss surgery, and men 50-69 who have undergone a Roux-en-Y gastric bypass.
- Bypassing the duodenum has caused metabolic bone disease in some patients, resulting in bone pain, loss of height, humped back and fractures of the ribs and hip bones. All of the deficiencies mentioned above, however, can be managed through proper diet and vitamin supplements.
- Chronic anemia due to vitamin B12 deficiency can occur. This can usually be managed with vitamin B12 pills or injections.
- When removing or bypassing the bottom of the stomach, a condition known as dumping syndrome can occur as a result of rapid emptying of the stomach contents into the small intestine. This can be triggered when too much sugar or fat is consumed. Symptoms can be extremely unpleasant and can include nausea, weakness, sweating, faintness and, on occasion, diarrhea after eating.
- In some cases, the effectiveness of the procedure may be reduced if the stomach pouch is stretched due to chronic overeating.
- Rerouting the bile, pancreatic and other digestive juices beyond the stomach can cause (via Roux-en-Y gastric bypass) intestinal irritation and ulcers if patients smoke or take NSAIDs.
- The lower stomach pouch and segments of the small intestine cannot be easily visualized using x-ray or endoscopy if problems such as ulcers, bleeding or malignancy should occur.
Vertical Sleeve Gastrectomy
The vertical sleeve gastrectomy is a procedure that limits the amount of food you can eat by reducing the size of your stomach, resulting in a feeling of fullness after eating a much smaller amount of food. Removal of this part of the stomach also decreases the level of a powerful hunger hormone. In some cases, vertical sleeve gastrectomy is used as the first step before gastric bypass. Then, in the second step, the surgeon attaches a section of the small intestine directly to the stomach pouch, which allows food to bypass a portion of the small intestine.
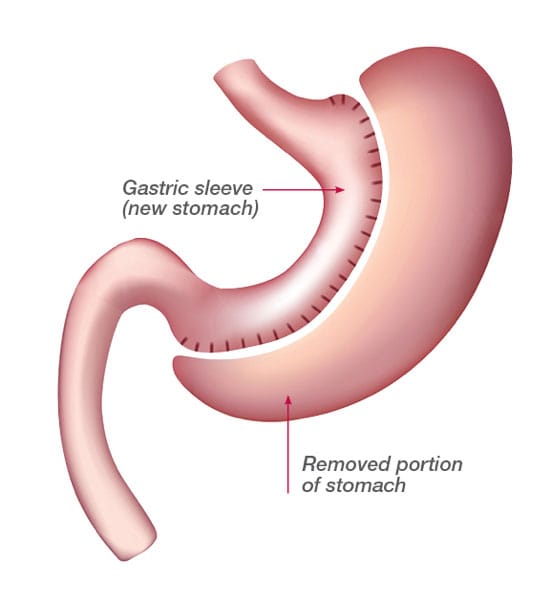
- The surgeon creates a small stomach “sleeve” using a stapling device. This sleeve will typically hold 50 mL to 150 mL and is about the size of a banana. The rest of the stomach is removed.
- This procedure induces weight loss in part by restricting the amount of food (and therefore calories) that can be eaten without bypassing the intestines and absorbed.
Advantages
- Limits the amount of food that can be eaten at a meal.
- Establishes a new, lower body fat set point.
- Food passes through the digestive tract in the usual order, thus there is less malabsorption of vitamins and minerals. This decreases the risk of some nutrient deficiencies.
- In clinical studies, patients lost an average of 66% of their excess weight.
- The procedure is shown to help resolve high blood pressure (49%), obstructive sleep apnea (60%), and to help improve type 2 diabetes (45%) and high cholesterol (77%).
Risks
In addition to the general risks of surgery, other risks include:
- Staple the leak
- Ulcers
- Dyspepsia
- Esophageal dysmotility
- The procedure is irreversible.
Laparoscopic Surgery
Laparoscopic surgery is a minimally invasive technique used in a wide variety of general surgeries, including bariatric and metabolic surgery. Many bariatric surgeons have received the necessary training to perform laparoscopic bariatric surgeries and offer patients this less invasive surgical option.
When a laparoscopic operation is performed, a small video camera is inserted into the abdomen. The surgeon views the procedure on a separate video monitor. Most laparoscopic surgeons believe this offers better visualization and access to key anatomical structures.
The camera and surgical instrument are inserted through small incisions made in the abdominal wall. This approach is considered less invasive because it replaces the need for one long incision to open the abdomen. Benefits, as compared with open surgery, may include a marked decrease in surgery related discomfort, reduced time in hospital and hospital costs, and an earlier return to a full, productive lifestyle.
Laparoscopic procedures for bariatric surgery use the same principles as open surgery and produce similar excess weight loss results, however, not all patients are candidates for this approach.