Patient receives hospital care at home, surrounded by family and field nurses and directed by a physician
Jul 29, 2020
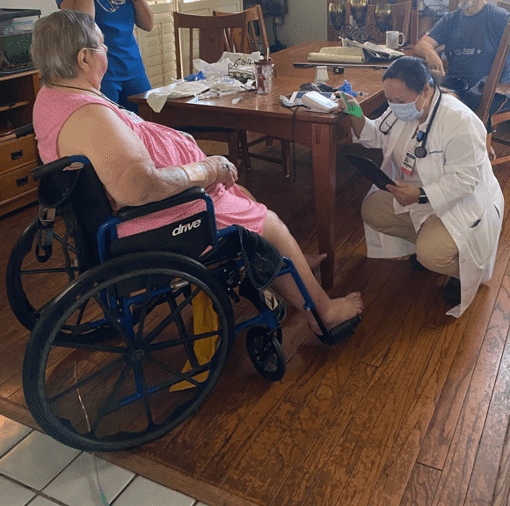
Sitting in her wheelchair with a nurse practitioner kneeling in front of her and a registered nurse by her side, Lois Heavrin, 89, received care and medication, just like in the hospital – but this hospital is in her home. Being hospitalized at home means the patient is surrounded by their family while receiving hospital care brought to them.
Heavrin was among the first patients to take advantage of the Adventist Health Hospital@Home program, which launched in May 2020 to help with hospital bed capacity in the event of a surge of COVID-19 patients. This innovative program is a partnership between Adventist Health and Medically Home and Huron to use virtual technology, such as iPads and monitors, to safely care for patients from the comfort of their homes.
In addition to field nurses and providers, the program features 24/7 virtual monitoring from a remote telemedical command center staffed by specially trained Adventist Health doctors and nurses.
“I was worried about COVID-19, so when this virtual hospital came up, it sounded like the ideal situation,” says Heavrin. “It was really nice that I could receive care and be at home with my son and daughter-in-law.”
Heavrin was discovered to be a good candidate for the program, after arriving at the Adventist Health Hanford Emergency Department due to swelling from cellulitis, which is a bacterial skin infection. She also suffers from congestive heart failure, which makes it hard for her to breathe.
When patients are admitted to the emergency room, nurses in the Adventist Health Hospital@Home command center receive their information and determine if they meet the criteria for the program. If the patient’s provider approves, a virtual visit is coordinated, and the virtual hospital is dispatched immediately. An information technology team member is deployed to the home, bringing and installing a tablet, telephone, blood pressure monitor, and scale. The team also installs back-up power and WiFi to expand wireless capacity to ensure the patient remains in communication with their care team at all times.
In the event of an emergency, the patient also has a personal emergency device and can click a button to contact a nurse for help.
During her virtual visit, Heavrin was able to speak with her doctor through the iPad and have blood drawn and in-home injections administered by her field nurses.
“The nurses were so kind and efficient. I thought it was a tremendous experience,” she says.
Medical command centers are active in Hanford and Ukiah to assist patients in Bakersfield, Clear Lake, Glendale, Los Angeles, Mendocino County, Simi Valley, and Hanford.
“We are fortunate enough to have a command center positioned in our hospital, with skilled nurses and doctors at the helm,” says Andrea Kofl, president of Adventist Health in the Central Valley. “Our mission to live God’s love inspires us to innovate care to fit our patients’ needs and situations.
More information about Adventist Health’s virtual hospital may be found by visiting: AdventistHealth.org/VirtualHospital.


